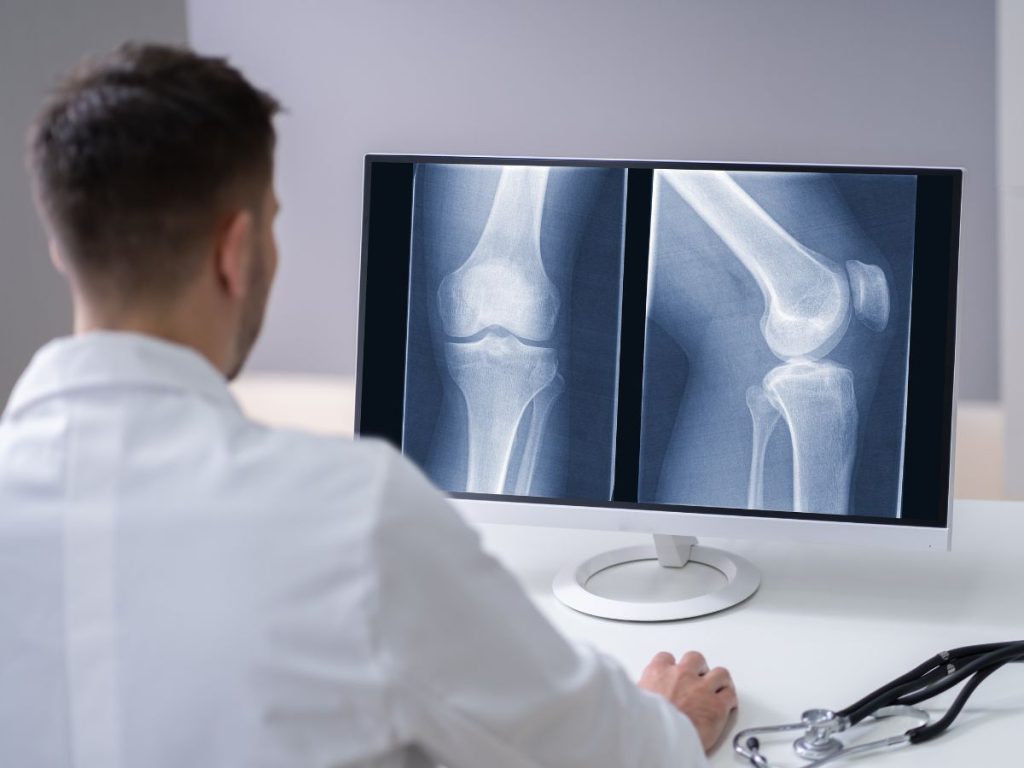
Imaging techniques like X-rays and MRIs often miss essential details about injuries, especially soft tissue damage. X-rays can’t effectively show muscle, ligament, or tendon injuries, while MRIs might overlook subtle tears. Plus, the timing of the scan can impact what’s visible—swelling can obscure true injury details. To get a complete picture, combining imaging results with thorough clinical assessments is critical. There’s much more to explore regarding effective injury diagnosis and treatment options.
Key Takeaways
- Imaging techniques like X-rays and MRIs have limitations, often missing soft tissue damage or subtle injuries critical for accurate diagnosis.
- X-rays primarily reveal bone fractures, leaving soft tissue injuries, such as muscle tears and ligament sprains, undetected.
- MRIs may overlook subtle tears due to anatomical variations and imaging specificity, leading to potential misdiagnosis.
- Timing of imaging can significantly affect results; delayed imaging may alter injury appearance while early imaging may misrepresent inflammation.
- Combining imaging with thorough clinical assessments and patient history enhances diagnostic accuracy and reveals insights beyond what imaging alone can provide.
Understanding the Limitations of Imaging in Injury Diagnosis
While imaging techniques like X-rays and MRIs are invaluable tools in diagnosing injuries, they’ve their limitations. You might assume that these images provide a complete picture, but that’s a common misconception.
For instance, X-rays excel at showing bone fractures but often miss soft tissue damage, which can lead to misleading conclusions. Similarly, MRIs, while detailed, can sometimes present false positives or miss subtle injuries altogether.
This can impact diagnostic accuracy, making it essential to evaluate clinical assessments alongside imaging results. Relying solely on images can lead to misdiagnosis or inappropriate treatment plans.
It’s vital to communicate openly with your healthcare provider about your symptoms and concerns. Understanding these limitations helps you and your doctor make informed decisions, ensuring a more accurate diagnosis and effective treatment strategy for your injury.
The Limitations of X-Rays for Soft Tissue Injuries
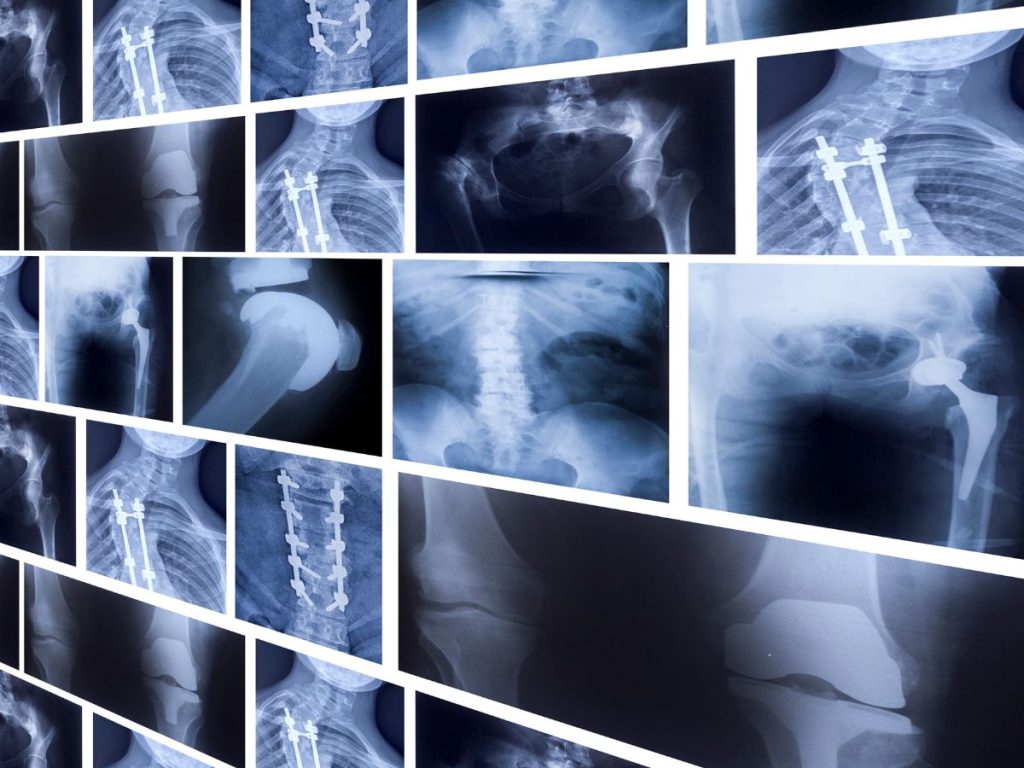
Imaging techniques like X-rays are often the first step in diagnosing injuries, but they fall short when it comes to soft tissue damage. While X-rays excel at revealing bone fractures, they can’t effectively show soft tissue injuries, such as muscle tears, ligament sprains, or tendon damage.
This limitation can lead to incomplete injury assessments, leaving you with unresolved pain or dysfunction. When you’re experiencing discomfort, relying solely on X-rays mightn’t provide the full picture.
Soft tissues don’t absorb X-rays the same way bones do, making it challenging to identify the extent of your injury. As a result, your healthcare provider may miss critical details that could impact your treatment plan.
Understanding these limitations is essential for steering your recovery. If you suspect a soft tissue injury, discussing further imaging options, like ultrasounds or MRIs, can lead to a more accurate diagnosis and effective management of your condition.
Why MRIs May Miss Key Injury Details?
Although MRIs are often considered the gold standard for diagnosing soft tissue injuries, they can still miss essential details. One reason is the inherent MRI limitations, including imaging specificity. Certain injuries, especially those with complexities, may not be clearly visualized. For example, subtle tears or micro-injuries can evade detection, leaving you without a complete picture.
Additionally, anatomical variations among individuals can complicate interpretation. What’s normal for one person may appear as an issue for another, leading to misdiagnosis.
While contrast agents can enhance soft tissue visualization, they aren’t always used, limiting the clarity of the image.
Ultimately, even with advanced technology, MRIs mightn’t capture every detail of your injury, which is why a thorough assessment—including clinical evaluation—is essential for effective treatment. Understanding these factors helps you appreciate the limitations of MRIs in addressing your specific injury.
How Timing Affects Imaging Results
Understanding when to get imaging can greatly impact the results you receive. The timing of your imaging plays a vital role in accurately evaluating your injury. If you wait too long, the injury progression might alter what the imaging reveals. For example, an MRI taken shortly after an injury can show soft tissue damage, while one taken days or weeks later might miss subtle details or indicate healing that’s already begun.
Conversely, rushing into imaging too soon can lead to misleading results, as inflammation or swelling might obscure the true nature of your injury.
It’s important to balance imaging timing with the understanding that injuries evolve. Working closely with your healthcare provider guarantees that the imaging you receive reflects the current state of your injury, giving you the best chance for an accurate diagnosis and effective treatment.
How Swelling Affects Imaging Accuracy
Swelling can greatly distort imaging results, making it important to assess its effects when evaluating injuries. When you experience swelling, the increased fluid can obscure underlying tissues, leading to imaging distortion. This distortion can mask fractures, tears, or other injuries that require accurate diagnosis.
Here’s a quick overview of how swelling affects different imaging techniques:
| Imaging Technique | Swelling Effects |
| X-ray | May hide fractures behind fluid |
| MRI | Can obscure soft tissue details |
| CT Scan | Fluid may mimic other conditions |
| Ultrasound | Increased fluid can reduce clarity |
| Bone Scan | Swelling may lead to false positives |
Understanding these swelling effects is significant for accurate injury assessment. If you’re dealing with swelling, it’s important to communicate this to your healthcare provider to guarantee the right imaging approach is taken.
Understanding Healing Phases and Their Impact on Imaging
As your body begins to heal after an injury, the different phases of healing can greatly influence imaging outcomes. Understanding the healing timeline is essential because each phase—acute, repair, and remodeling—can affect what imaging technology reveals.
In the acute phase, swelling and inflammation can obscure details, making it hard to identify the full extent of damage. As you move into the repair phase, new tissue forms, which might show up on an MRI or ultrasound, but it may not reflect the underlying severity.
Finally, during the remodeling phase, the body strengthens and reorganizes tissue, potentially leading to clearer images. However, even in this phase, imaging mightn’t capture all nuances of the injury.
Recognizing these phases helps you appreciate why imaging results can sometimes be misleading and underscores the importance of a thorough evaluation for a complete understanding of your injury.
The Importance of Clinical Assessment in Injury Diagnosis
Imaging plays an essential role in diagnosing injuries, but it shouldn’t be the sole focus. Relying solely on scans can lead to missed nuances that only a thorough clinical assessment can reveal. Your healthcare provider’s clinical intuition is vital; it guides them in understanding your symptoms and how they align with your injury.
While imaging provides valuable information, it can’t capture everything. For instance, a physical examination can uncover tenderness, swelling, or range-of-motion limitations that imaging might overlook. This hands-on evaluation greatly boosts diagnostic accuracy, ensuring you receive the correct treatment.
Listening to your concerns and observing your body’s reactions offers insights that images alone can’t provide. By combining clinical assessment with imaging, you empower your healthcare provider to make informed decisions that lead to better recovery outcomes.
Always remember, a well-rounded approach is key to effective injury diagnosis.
What Common Misdiagnoses Occur From Over-Reliance on Imaging?
When you rely too heavily on imaging, you might miss vital soft tissue injuries that don’t show up on scans.
It’s easy to overlook functional issues that could be impacting a patient’s recovery.
Understanding these pitfalls can help improve diagnostic accuracy and treatment outcomes.
Soft Tissue Injuries Missed
While advanced imaging techniques have revolutionized diagnostics, over-reliance on these tools can lead to missed soft tissue injuries. You might encounter several common misdiagnoses, which can complicate your recovery:
- Tendon injuries: Often overlooked, these can manifest as pain without clear imaging evidence.
- Ligament sprains: Subtle sprains may not show up on scans, leading to incorrect assessments.
- Fascia damage: This tissue can be affected without showing significant changes on imaging techniques.
These diagnostic challenges highlight the importance of combining imaging with thorough assessment methods.
Understanding various injury patterns and their clinical implications is essential for effective rehabilitation strategies. By not solely depending on imaging, you can better navigate your recovery journey.
Functional Issues Overlooked
Over-relying on imaging can lead to overlooked functional issues that greatly affect your recovery. When doctors focus solely on scans, they might miss important aspects of how your body moves and functions.
For instance, a sprain might show no significant damage on an MRI, yet you could still experience pain and instability. Without proper functional assessments, these issues may remain unaddressed, leading to misdiagnoses.
This oversight can hinder your rehabilitation strategies, causing prolonged discomfort and delayed healing. It’s essential to combine imaging with hands-on evaluations and movement analysis to gain a complete picture of your injury.
Techniques to Complement Imaging in Injury Diagnosis
When diagnosing injuries, you can’t rely solely on imaging.
Incorporating physical examination techniques and understanding the patient’s history are essential for accurate assessments.
These complementary approaches help reveal insights that images alone might miss.
Physical Examination Techniques
A thorough physical examination is essential in diagnosing injuries, as it provides critical insights that imaging techniques alone may miss.
To effectively assess an injury, consider these key techniques:
- Palpation Techniques: Gently pressing on specific areas helps identify tenderness, swelling, or abnormalities that imaging might overlook.
- Range Assessment: Evaluating the range of motion allows you to pinpoint restrictions or pain that indicate underlying issues.
- Functional Testing: Observing how an injury affects movement can reveal critical information about severity and impact on daily activities.
Patient History Importance
While imaging provides valuable insights into injuries, understanding a patient’s history is equally essential for accurate diagnosis.
Patient narratives offer a rich context that imaging alone can’t capture. When you listen to a patient describe their symptoms, you gather critical details about the onset, duration, and nature of their pain.
This historical context can reveal patterns or triggers that guide your diagnosis. For instance, a past injury might predispose them to a current problem, or their lifestyle may contribute to ongoing issues.
By integrating these personal stories with imaging results, you create a more thorough view of the injury.
Ultimately, this combination leads to better treatment plans and improved outcomes for your patients.
Frequently Asked Questions
Can Imaging Detect All Types of Injuries Accurately?
No, imaging can’t detect all injury types accurately due to imaging limitations. Some injuries, like soft tissue damage or subtle fractures, may not show up clearly, leaving you with incomplete information about your condition.
How Do Imaging Techniques Differ in Effectiveness?
Imaging techniques differ markedly. MRI has limitations in detecting certain injuries, while CT scans offer advantages in speed and detail. Ultrasound is great for soft tissues, but X-rays can sometimes miss fractures or subtle issues.
What Role Does a Patient’s History Play in Diagnosis?
A patient’s history considerably enhances diagnostic accuracy. By sharing detailed patient narratives, you help healthcare providers understand symptoms and patterns, leading to more effective assessments and tailored treatment plans for your specific condition.
Are There Alternative Methods to Assess Injuries Besides Imaging?
Yes, you can assess injuries through a thorough physical examination and various diagnostic tools. Techniques like palpation, range of motion tests, and functional assessments often provide valuable insights that imaging might miss.
How Often Should Imaging Be Repeated During Recovery?
You should repeat imaging as needed during recovery, usually every few weeks, to monitor progress. Adjust the imaging frequency based on your symptoms and the healthcare provider’s recommendations for effective recovery assessment.
Final Thoughts
Imaging can be an important part of the diagnostic process, but it does not always tell the whole story. Soft tissue damage, inflammation, and injuries in the early or changing stages of healing may not appear clearly on an X-ray or MRI, which is why symptoms should never be dismissed simply because imaging looks normal. A complete evaluation should always consider both what the images show and what your body is telling you.
At Agnew Family Wellness, we take a comprehensive approach through personalized accident care and advanced chiropractic care to help uncover the source of pain and support full recovery. If you are still dealing with symptoms after an accident, even when imaging does not show the full extent of the injury, do not ignore what you are feeling. Visit our blog for more recovery guidance or contact us today to take the next step toward lasting healing.